HLA Typing (Human Leukocyte Antigen)
HLA Typing, or human leukocyte antigen typing, is a medical test that identifies the specific alleles (gene variants) of the human leukocyte antigen system. HLA genes are found on chromosome 6 and play a crucial role in the immune system. They encode proteins that are responsible for presenting antigens (foreign substances like bacteria or viruses) to the immune system, allowing the immune system to recognize and respond to these invaders.
There are two main classes of HLA genes:
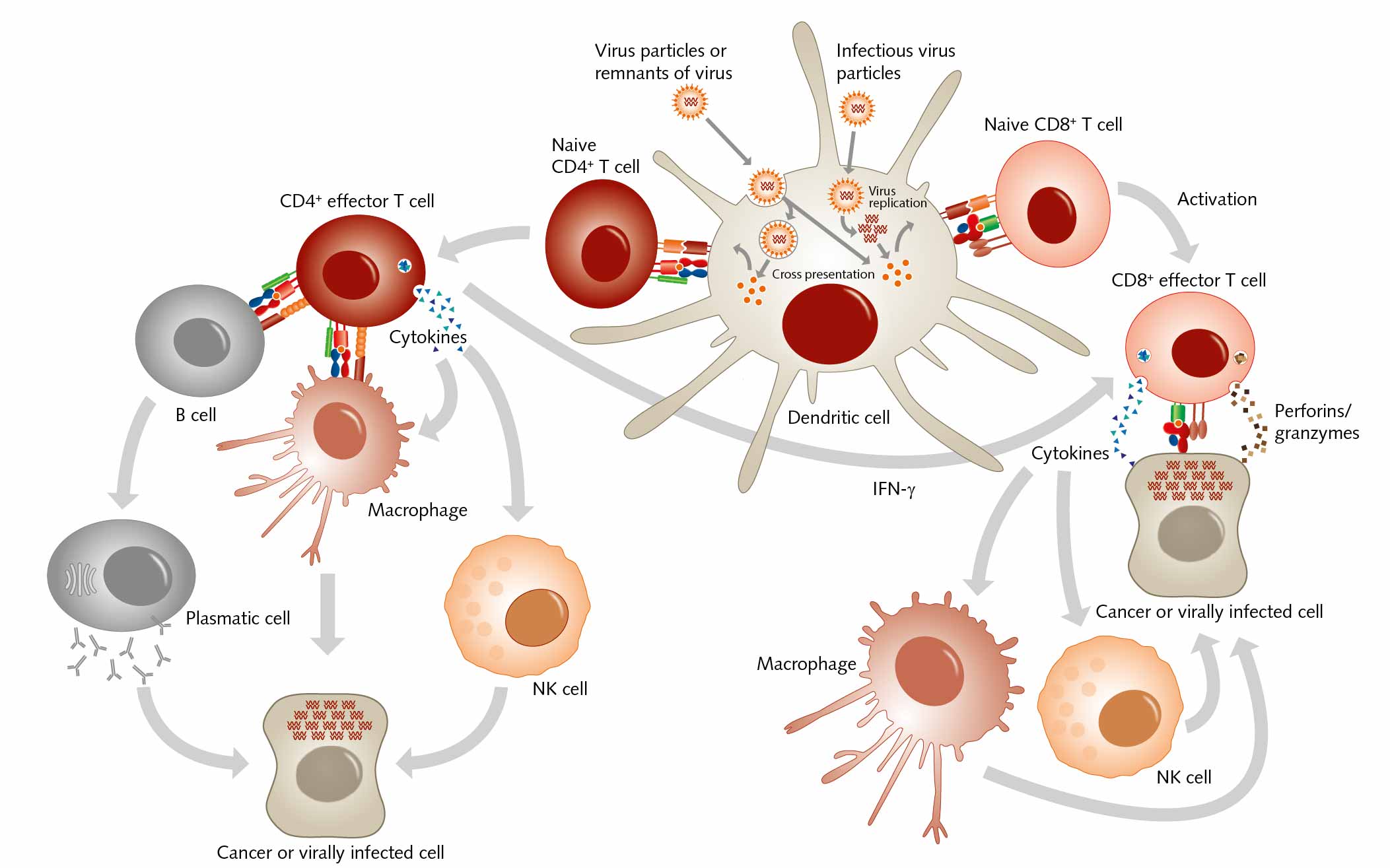
- Class I HLA genes (HLA-A, HLA-B, and HLA-C): These genes encode proteins that are present on the surface of nearly all nucleated cells in the body. They present antigens from inside the cell to cytotoxic T cells, which can then eliminate infected or abnormal cells.
- Class II HLA genes (HLA-DP, HLA-DQ, and HLA-DR): These genes encode proteins that are mainly found on the surface of antigen-presenting cells such as dendritic cells, macrophages, and B cells. They present antigens from outside the cell to helper T cells, which help coordinate the immune response.
HLA typing is important for several reasons:
- Organ Transplants: Matching HLA types between donors and recipients is crucial in organ transplantation to minimize the risk of graft rejection. A closer HLA match between the donor and recipient reduces the likelihood of the recipient’s immune system attacking and rejecting the transplanted organ.
- Disease Associations: Certain HLA types are associated with an increased risk of developing specific autoimmune diseases, such as type 1 diabetes, rheumatoid arthritis, and celiac disease. Understanding a person’s HLA type can help diagnose and manage these conditions.
- Drug Allergies: Some drug hypersensitivity reactions are associated with specific HLA alleles. Knowing a patient’s HLA type can help healthcare providers choose medications that are less likely to cause adverse reactions.
- Forensic Genetics: HLA typing can be used in forensic science to help identify individuals or determine paternity.
- Anthropology and Population Genetics: HLA typing is also used in population genetics and anthropology to study human genetic diversity and migration patterns.
Purpose of HLA Typing:
Human leukocyte antigen (HLA) typing is a crucial medical procedure used to determine an individual’s unique HLA profile. The purpose of HLA typing is primarily related to its role in the immune system and its significance in various medical contexts:
- Organ and Tissue Transplantation:
- Matching HLA types between the donor and recipient is crucial for successful organ and tissue transplantation. A close HLA match reduces the risk of graft rejection, where the recipient’s immune system attacks the transplanted organ or tissue.
- Bone Marrow and Stem Cell Transplantation:
- HLA typing is essential for finding suitable donors for bone marrow and hematopoietic stem cell transplants. A close HLA match minimizes the risk of graft-versus-host disease (GVHD), where donor immune cells attack the recipient’s tissues.
- Blood Transfusions:
- HLA matching is considered for blood transfusions, particularly for patients who require frequent transfusions or have developed antibodies against specific HLA antigens. Matching HLA can help reduce adverse reactions and complications.
- Autoimmune Diseases:
- Understanding an individual’s HLA type can provide insights into their susceptibility to autoimmune diseases. Certain HLA alleles are associated with an increased risk of developing autoimmune disorders such as type 1 diabetes, rheumatoid arthritis, and celiac disease.
- Disease Associations:
- HLA typing is used in medical research to study associations between specific HLA alleles and various diseases, including infectious diseases like HIV and autoimmune conditions. This information can aid in understanding disease mechanisms and developing targeted treatments.
- Pharmacogenomics:
- Some HLA alleles are associated with drug sensitivity and adverse drug reactions. HLA typing can help guide medication selection to minimize the risk of adverse reactions and optimize treatment outcomes.
- Forensic Science:
- HLA typing is sometimes used in forensic science to help identify individuals in criminal cases or mass disasters when DNA testing is not possible or insufficient.
- Anthropology and Population Genetics:
- Studying HLA diversity among populations provides insights into human evolutionary history and migration patterns. It can also be used to understand the genetic diversity of different populations.

HLA Typing for Transplants:
Here are some key points about HLA typing for transplants:
- HLA System: Human leukocyte antigens are proteins found on the surface of most cells in the human body. They are highly variable between individuals and are crucial for immune system recognition. There are two main classes of HLA molecules: Class I (HLA-A, HLA-B, and HLA-C) and Class II (HLA-DR, HLA-DQ, and HLA-DP).
- Matching: The goal of HLA typing is to find a donor whose HLA types closely match those of the recipient. A closer match reduces the risk of rejection because the immune system is less likely to recognize the transplanted organ as foreign.
- HLA Typing Methods: HLA typing can be performed using various techniques, including serological (antibody-based) methods, sequence-specific oligonucleotide (SSO) typing, and DNA-based methods like polymerase chain reaction (PCR) and DNA sequencing. The choice of method depends on the specific requirements of the transplant and the available resources.
- Family Members: When a suitable match cannot be found in the general population, family members, particularly siblings, are often the next best option because they are more likely to share HLA types due to their common genetic heritage.
- Molecular HLA Typing: Molecular HLA typing methods, such as PCR and DNA sequencing, provide high-resolution typing and can distinguish between closely related HLA alleles. This level of detail is essential for optimizing donor-recipient compatibility.
- Transplant Rejection: If there is a significant mismatch between the donor’s and recipient’s HLA types, the recipient’s immune system may recognize the transplanted organ as foreign and mount an immune response, leading to rejection. To prevent this, immunosuppressive medications are typically prescribed post-transplant to dampen the recipient’s immune response.
- Organ Transplants: HLA matching is particularly critical in solid organ transplants, such as kidney, liver, and heart transplants, where the recipient’s immune system must be carefully managed to avoid rejection.
- Bone Marrow Transplants: In bone marrow or stem cell transplants, HLA matching is crucial to prevent graft-versus-host disease (GVHD), a potentially life-threatening condition where the donor’s immune cells attack the recipient’s tissues.
- Registry Matching: National and international registries, such as the National Marrow Donor Program (NMDP) for bone marrow donors, help match donors with recipients based on HLA typing. These registries maintain a database of potential donors and recipients, increasing the chances of finding suitable matches.
Other Types of HLA Testing:
While the most common type of HLA testing is HLA typing for organ transplantation compatibility, several other types of HLA testing serve different purposes:
- HLA-B27 Testing: This test specifically looks for the presence of the HLA-B27 antigen. It’s primarily used to diagnose conditions like ankylosing spondylitis, reactive arthritis, and other autoimmune disorders. The presence of HLA-B27 is associated with an increased risk of these conditions.
- HLA Cross-Matching: In organ transplantation, HLA cross-matching is performed to ensure compatibility between the donor and recipient. It helps identify if there are antibodies in the recipient’s blood that react with the donor’s HLA antigens, which could lead to organ rejection.
- HLA Antibody Testing: This test detects the presence of antibodies in a recipient’s blood that might react with HLA antigens. It is crucial to assess the risk of hyperacute rejection in organ transplantation.
- HLA Panel Testing: HLA panels are used to identify a wide range of HLA antigens in a single test. These panels can be customized to look at specific HLA loci or a broader range of antigens. They are often used for research and population studies.
- HLA Class I and Class II Typing: HLA genes are categorized into Class I (HLA-A, HLA-B, and HLA-C) and Class II (HLA-DR, HLA-DP, and HLA-DQ). Testing can be done separately for each class, depending on the clinical need.
- HLA-DQ2 and HLA-DQ8 Testing: These specific tests are often used in the diagnosis of celiac disease, as individuals carrying the HLA-DQ2 or HLA-DQ8 genes are at a higher risk of developing the condition.
- HLA-B*5701 Testing: This test is important in HIV treatment, specifically when prescribing the drug abacavir (Ziagen). People with the HLA-B*5701 allele are at a higher risk of severe hypersensitivity reactions to this medication.
- HLA-DR Typing for Autoimmune Diseases: In certain autoimmune diseases, such as rheumatoid arthritis, specific HLA-DR alleles are associated with an increased risk. Testing for these alleles can aid in diagnosis and prognosis.
- HLA-DRB1 Testing for Multiple Sclerosis: Certain HLA-DRB1 alleles have been linked to an increased risk of developing multiple sclerosis. Testing for these alleles can provide additional information for diagnosis and risk assessment.
- HLA-DQ Typing for Gluten Sensitivity: In addition to celiac disease, some individuals may have non-celiac gluten sensitivity. HLA-DQ typing can help rule out celiac disease and support the diagnosis of gluten sensitivity.
What Is the HLA System?
The HLA system, or Human Leukocyte Antigen system, is a crucial component of the human immune system. It is a group of proteins found on the surface of most cells in the body, except red blood cells. HLA molecules play a central role in the regulation of the immune system and in the body’s ability to distinguish between its cells and foreign invaders, such as bacteria, viruses, and transplanted tissues or organs.

The Process of HLA Typing:
Human Leukocyte Antigen (HLA) typing is a method used to identify and characterize the specific HLA genes and alleles present in an individual’s immune system. HLAs are proteins that play a crucial role in immune responses, particularly in recognizing and distinguishing self from non-self cells. HLA typing is important in various medical contexts, such as organ and tissue transplantation, autoimmune disease diagnosis, and understanding the genetic basis of certain diseases. Here’s an overview of the process of HLA typing:
- Sample Collection: A sample of blood, saliva, or tissue is collected from the individual. Blood is the most common sample type used for HLA typing.
- DNA Extraction: The collected sample is processed to extract DNA. DNA contains the genetic information required for HLA typing.
- Polymerase Chain Reaction (PCR): Specific regions of the HLA genes are amplified using PCR. PCR is a technique that generates millions of copies of a specific DNA segment, allowing for further analysis.
- DNA Sequencing or PCR-SSP: There are different methods to perform HLA typing, and the choice depends on the level of detail needed. The most accurate method involves DNA sequencing, which provides the complete genetic sequence of the HLA genes. Another common method is Polymerase Chain Reaction–Sequence-Specific Primers (PCR-SSP), which identifies specific known alleles based on the pattern of amplified DNA fragments.
- Data Analysis: The sequencing or PCR-SSP results are analyzed to determine the specific alleles present in the individual’s HLA genes. This involves comparing the obtained sequences or patterns with a reference database of known HLA alleles.
- HLA Typing Resolution: HLA genes are highly polymorphic, meaning they have numerous different alleles in the population. These alleles are classified into different levels of resolution (low, intermediate, and high). Low-resolution typing identifies broad allele groups, while high-resolution typing identifies specific alleles. High-resolution typing is usually necessary for transplantation, as certain allele differences can significantly affect compatibility.
- HLA Nomenclature: HLA alleles are named based on a standardized nomenclature system. Each allele is identified by a combination of gene loci (such as HLA-A, HLA-B, HLA-DRB1, etc.), a series of numbers and/or letters denoting the specific allele, and additional information about variations.
- Reporting Results: The final HLA typing results are reported to the requesting healthcare provider or laboratory. These results are important for matching organ and tissue donors with recipients, diagnosing autoimmune diseases, studying disease associations, and conducting research on immune-related conditions.
Is HLA Typing the Same as Blood Typing?
No, HLA typing is not the same as blood typing. These are two distinct processes that provide different types of information about an individual’s biology.
- Blood Typing: Blood typing, also known as blood group typing, determines an individual’s blood group or blood type. The most common blood typing system is the ABO system, which classifies blood into four major types: A, B, AB, and O. Another important blood group system is the Rh factor, which classifies blood as Rh-positive or Rh-negative. Blood typing is crucial for blood transfusions to ensure compatibility between the donor’s blood and the recipient’s blood.
- HLA Typing: HLA stands for Human Leukocyte Antigen. HLA typing is a process that identifies specific proteins (antigens) on the surface of white blood cells (leukocytes). These HLA proteins play a critical role in the immune system, particularly in the recognition of self from non-self. HLA typing is essential for various medical purposes, such as organ transplantation and the treatment of autoimmune diseases. It helps ensure compatibility between the donor’s and recipient’s HLA types to reduce the risk of rejection in organ transplant cases.
In summary, blood typing primarily deals with identifying an individual’s blood group (ABO and Rh) and is important for blood transfusions. HLA typing, on the other hand, focuses on identifying specific proteins in white blood cells and is crucial for organ transplantation and immune-related diseases. While both involve understanding aspects of an individual’s biology, they serve different medical purposes.
Interpreting Results of HLA Typing:
HLA genes encode proteins that play a key role in the immune system’s ability to distinguish between self and foreign substances. Understanding HLA typing results is essential for matching donors and recipients in transplantation and for studying associations with diseases. Here’s how to interpret HLA typing results:
- HLA Alleles: HLA genes have many different alleles, and individuals inherit two copies of each HLA gene, one from each parent. The results will typically include information about the specific alleles detected for each HLA gene. For example, an HLA-A typing might show alleles like HLA-A02:01 and HLA-A11:01.
- Specific Loci: HLA genes are divided into class I (HLA-A, HLA-B, HLA-C) and class II (HLA-DR, HLA-DP, HLA-DQ) loci. The results will specify which loci were tested and the alleles detected for each locus.
- Allelic Match: In the context of transplantation, a good match involves compatibility between the donor’s and recipient’s HLA alleles. The more closely the alleles match, the lower the risk of graft rejection. It’s essential to assess compatibility at all relevant loci.
- Expression of Proteins: HLA alleles encode proteins that are expressed on the surface of cells. The specific combination of HLA proteins in an individual’s cells determines their tissue type. In transplantation, a closer match in tissue type is preferred to reduce the risk of graft-versus-host disease (GVHD).
- Heterozygosity: Since individuals inherit two copies of each HLA gene, they can be homozygous (both copies are the same) or heterozygous (the copies are different). Heterozygosity can be advantageous for transplantation since it increases the likelihood of finding a compatible donor.
- Linkage Disequilibrium: Sometimes, certain HLA alleles are found together more frequently than would be expected by chance. This is known as linkage disequilibrium. Understanding linkage disequilibrium can provide additional information about an individual’s HLA profile.
- Clinical Implications: In transplantation, the interpretation will depend on whether you’re looking at results for a donor or a recipient. For a donor, you want to find the closest match possible to reduce the risk of graft rejection. For a recipient, you want to assess their HLA type to find a compatible donor.
- Disease Associations: In research, HLA typing can be used to study associations between specific HLA alleles and diseases, particularly autoimmune diseases like rheumatoid arthritis or celiac disease. Researchers look for patterns suggesting that certain alleles increase or decrease disease susceptibility.
- Population Frequencies: HLA alleles vary in frequency among different populations. Knowledge of population-specific HLA allele frequencies can be useful in transplantation and disease association studies.
- Nomenclature: HLA alleles are named according to a standardized nomenclature system that reflects their genetic sequences. Understanding this nomenclature is essential for accurately interpreting results.
Interpreting HLA typing results can be complex, and it’s often done by specialists in the field. In transplantation, close matching is crucial for success, while in disease association studies, the focus may be on identifying patterns and correlations.
How Many HLA Matches Do You Need?
The number of HLA (Human Leukocyte Antigen) matches required depends on the context in which HLA matching is being considered. HLA matching is primarily important in the fields of organ transplantation and bone marrow transplantation (hematopoietic stem cell transplantation). Here’s a general overview of how many HLA matches are typically required in these contexts:
Organ Transplantation
- Kidney Transplant: For kidney transplantation, the best outcomes are generally achieved with a close HLA match. A perfect HLA match (6 out of 6 antigens matching) is ideal but not always necessary. Many kidney transplants are successful with 4 to 6 HLA antigen matches.
Liver Transplant: HLA matching is less critical for liver transplantation compared to kidney transplantation. Generally, liver transplants can be successful with fewer HLA matches.
Bone Marrow Transplantation (Hematopoietic Stem Cell Transplantation)
- Related Donor: When the donor is a close relative (e.g., a sibling), a higher level of HLA matching is ideal. A perfect match (10 out of 10 HLA alleles matching) is often sought for the best outcomes.
- Unrelated Donor: When the donor is unrelated to the recipient, finding a perfect match can be more challenging. However, the closer the HLA match, the better the chances of a successful transplant. Many transplant centers aim for at least 8 out of 8 HLA antigen matches for unrelated donor transplants.
It’s important to note that HLA matching is just one factor considered when evaluating organ or bone marrow transplant compatibility. Other factors such as blood type, antibody levels, and overall health are also taken into account.
The specific requirements for HLA matching can vary from one transplant center or institution to another, and advancements in transplantation techniques and immunosuppressive medications can also influence the degree of matching required. Therefore, patients and potential donors need to consult with their healthcare providers and transplant teams for individualized guidance regarding HLA matching requirements for their specific situation.


[…] after a baby is born. It is collected shortly after birth and is rich in stem cells, specifically hematopoietic stem cells, which can develop into various types of blood cells, including red blood cells, white […]
[…] Trials: In some cases, Complement C3 tests are used in clinical research or trials to study the complement system’s role in various diseases and to develop new […]
[…] is not well-documented due to its microscopic nature and the absence of fossils. However, based on genetic studies, it is believed to be an ancient organism that diverged early in the eukaryotic […]