Measles virus (Transmission)
Measles virus, The measles virus, scientifically known as Measles morbillivirus, is a highly contagious virus that belongs to the Paramyxoviridae family. It causes the disease known as measles, which primarily affects humans. Measles is characterized by a high fever, a distinctive red rash, and other symptoms such as cough, runny nose, and conjunctivitis (pink eye).
Transmission:
The measles virus is primarily transmitted from person to person through respiratory droplets. Here’s how the transmission typically occurs:
- Infected Person: An individual infected with the measles virus can spread the virus to others during the early stages of infection, even before they start showing symptoms.
- Coughing and Sneezing: When an infected person coughs or sneezes, they release tiny respiratory droplets into the air. These droplets can contain the measles virus if the person is infected.
- Airborne Transmission: The virus can remain suspended in the air for some time. If someone inhales these infected droplets or comes into contact with surfaces or objects contaminated with these droplets, they can become infected.
- Close Contact: Measles is highly contagious, and close contact with an infected person is a significant risk factor for transmission. Being in the same room as an infected individual, especially in confined spaces, increases the likelihood of transmission.
- Direct Contact: The virus can also spread through direct contact with respiratory secretions or the saliva of an infected person. This can occur through activities such as kissing, sharing utensils or drinking glasses, or touching surfaces contaminated with the virus and then touching the face.
- Infectious Period: Infected individuals are contagious from a few days before the onset of symptoms and continue to be contagious for several days after the characteristic measles rash appears. This means that even if someone with measles doesn’t have a rash yet, they can still transmit the virus.
Symptoms:
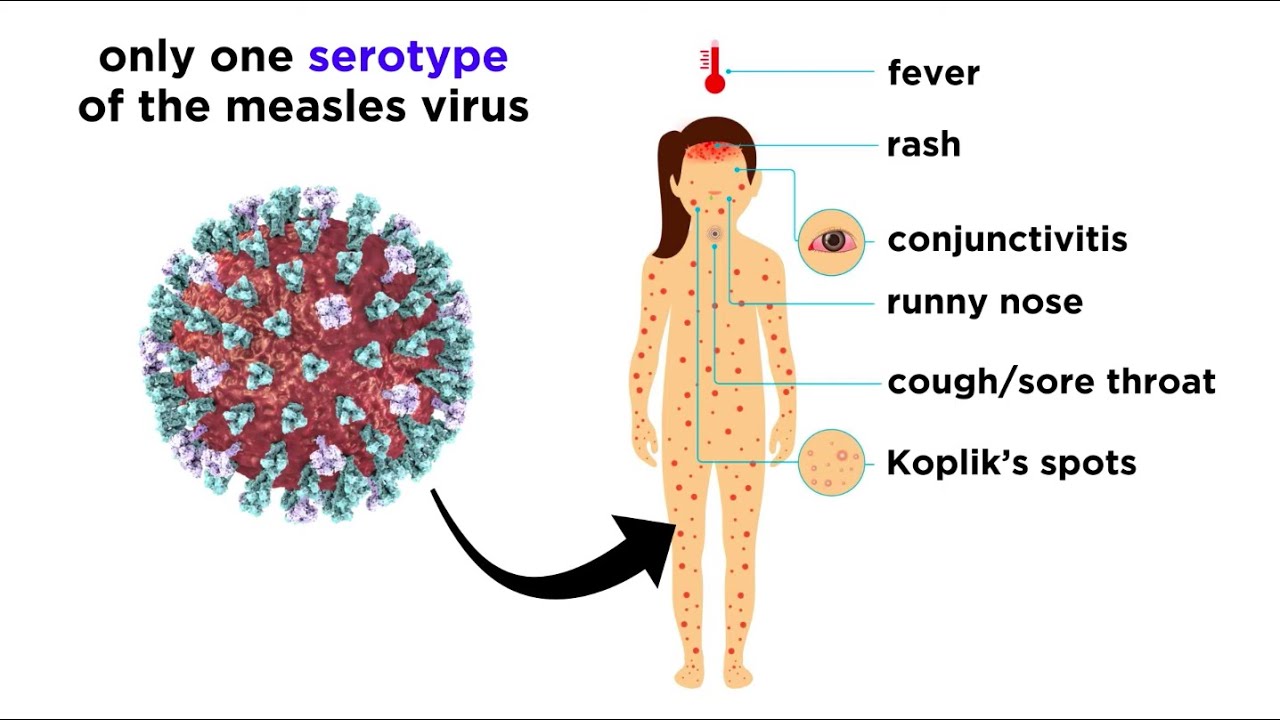
Measles, also known as rubeola, is a highly contagious viral infection caused by the measles virus. It can lead to a range of symptoms, which typically appear about 10-12 days after exposure to the virus. Common symptoms of measles include:
- Fever: Measles often begins with a high fever, which can spike to over 104°F (40°C).
- Cough: A persistent cough is a common symptom, often accompanied by a runny or stuffy nose.
- Sore Throat: Measles can cause a sore throat and discomfort when swallowing.
- Red Eyes (Conjunctivitis): Inflammation and redness of the eyes, along with sensitivity to light, may occur.
- Koplik’s Spots: Small white spots with bluish-white centers may appear inside the mouth on the inner lining of the cheeks. These are called Koplik’s spots and are characteristic of measles.
- Rash: A distinctive red or reddish-brown rash typically appears a few days after the initial symptoms. It often starts on the face and then spreads to other parts of the body. The rash consists of small, raised, and flat red spots that may merge as it spreads.
- Fatigue: Patients with measles often feel extremely tired and lethargic.
- Muscle Pain: Muscle aches and pains, as well as joint pain, are common.
- Loss of Appetite: A decreased appetite and nausea may accompany the illness.
- Complications: Measles can lead to serious complications, particularly in children and individuals with weakened immune systems. These can include pneumonia, ear infections, encephalitis (inflammation of the brain), and in severe cases, death.
Diagnosis:
Testing for the measles virus is typically done to confirm a suspected case of measles, monitor outbreaks, and assess immunity in certain populations. There are several different methods used for testing the measles virus, including:
- Serology (Blood Tests): Serological tests look for antibodies to the measles virus in a patient’s blood. Two types of antibodies are typically tested for:
- IgM Antibodies: IgM antibodies are produced in response to a recent measles infection. Detecting IgM antibodies in a blood sample can confirm an acute measles infection.
- IgG Antibodies: IgG antibodies indicate a past measles infection or immunity due to vaccination. A high level of IgG antibodies suggests immunity.
- Viral Culture: This involves attempting to grow the measles virus from a sample of the patient’s throat or urine. It is a less common method and is typically performed in specialized laboratories.
- Polymerase Chain Reaction (PCR): PCR is a highly sensitive molecular biology technique that can detect the genetic material (RNA) of the measles virus. It can be used to confirm an active measles infection, especially in the early stages.
- Throat Swabs: Throat swabs can be collected from a patient with suspected measles and tested for the presence of the virus. However, this method is less sensitive than PCR.
- Urine Tests: Urine samples can also be tested for the presence of the measles virus. Like throat swabs, this method is less sensitive than PCR.
- Saliva Tests: Some newer methods involve testing saliva for the measles virus. These tests may be more convenient, especially for children, and can be used in outbreak situations.
- IgE Antibody Test: IgE antibodies specific to the measles virus can also be detected in the blood. Elevated levels of these antibodies may suggest a recent or ongoing measles infection.
The choice of testing method depends on the stage of the illness and the resources available in the healthcare facility. PCR is often used for early diagnosis, while serological tests (IgM and IgG) can provide information about recent and past infections or vaccination history.
Risk:
The risk of contracting measles depends on various factors, including vaccination rates, population density, and travel patterns. Here are some key points to consider regarding the risk of measles:
- Vaccination Status: Measles can be prevented through vaccination with the measles, mumps, and rubella (MMR) vaccine. High vaccination rates within a population create “herd immunity,” which helps protect those who cannot be vaccinated, such as infants and individuals with weakened immune systems. When vaccination rates drop, the risk of outbreaks increases.
- Travel: Measles is a global disease, and international travel can contribute to the spread of the virus. Unvaccinated travelers may become infected abroad and bring the virus back to their home country, potentially sparking outbreaks.
- Outbreaks: Measles outbreaks can occur in areas with lower vaccination rates. These outbreaks can lead to increased transmission and pose a risk to unvaccinated individuals.
- Complications: Measles can lead to serious complications, including pneumonia, encephalitis (brain inflammation), and death. Infants, pregnant women, and individuals with weakened immune systems are at higher risk of severe complications.
- Symptoms: Measles symptoms typically include high fever, a characteristic rash, cough, runny nose, and red, watery eyes. It is highly contagious, and the virus can be transmitted through respiratory droplets from coughs and sneezes.
- Preventive Measures: Besides vaccination, other preventive measures include practicing good hygiene, such as handwashing, covering one’s mouth and nose when coughing or sneezing, and avoiding close contact with infected individuals.
- Global Efforts: The World Health Organization (WHO) has set ambitious goals to eliminate measles in various regions. These efforts involve increasing vaccination coverage and surveillance to detect and respond to outbreaks promptly.
Overall, the risk of measles can vary from one region to another and is influenced by factors such as vaccination rates, population immunity, and the presence of the virus in the community. Vaccination remains the most effective way to reduce the risk of contracting and spreading measles.



[…] Exposure to Contaminated Objects or Surfaces: It’s possible, though less common, for TB bacteria to persist on contaminated surfaces or objects for a short time. If someone touches these surfaces and then touches their mouth or nose, they can potentially introduce the bacteria into their respiratory system. However, direct person-to-person transmission through respiratory droplets is the primary mode of TB spread. […]
[…] Canker sores can develop on the inside of your cheeks, lips, tongue, gums, or the roof of your […]
[…] with someone who has the virus, or through contact with surfaces or objects contaminated with the virus, like doorknobs, handrails, or bathroom fixtures. People infected with norovirus can shed the virus […]
[…] Arthritis and joint pain are common symptoms in many autoimmune diseases associated with anti-ENA antibodies, such as SLE. […]
[…] Of Hepatitis Virus, Hepatitis is a deadly disease. Which slowly leads the patient to death. Hepatitis is an inflammation of the liver. There are six types of hepatitis which are as […]
[…] result of a dsDNA Ab test is usually considered together with a person’s medical history, signs and symptoms, and results of other autoantibody […]