Blood Banking & Blood Donation, The ABO, and Rhesus are the major (Clinically Significant) blood group antigens through almost 400 of them have been recognized. Given below are the more important blood group systems.
- ABO
- Rhesus
- Dekk
- MNS
- Lewis
- Kid
- Dully
- Lutheran
Slide ABO – Grouping:
- Prepare a 10% suspension in saline for the red blood cells to be tested.
- Mark the left side of a clean glass side “Anti-A” and the right side “Anti-B”.
- Add to the left side a drop of anti-A grouping serum and to the right side a drop of anti-B grouping serum.
- Next to the antisera drop, place 1 drop of 10% saline suspension with the anti-A serum, and with the other half mix the red cell suspension with the anti-B serum.
- With one-half of an applicator stick, mix the red cell suspension with the anti-A serum, and with the other half mix the red cell suspension with the anti-B serum.
- Gently rock the slide back and forth and observe the mixture for one minute unless agglutination occurs earlier.
- Agglutination will indicate that particular blood group where the antiserum is added.
- Mix serum and red cells and distribute them over a large area of the slide.

Rh Group (Slide Test):
- On a labeled glass slide place 1 drop of anti-RH serum (IgG).
- To the drop of antiserum add 2 drops of whole blood.
- Gently rock the slide back and forth and observe for agglutination.
- Gently rock the slide back and forth and observe for agglutination. 5. Observe the test for 2 minutes unless agglutination occurs earlier.
| Blood Group | Antigens | Antibodies | Can Get Blood From | Cannot Get Blood From |
| A | A | Anti-B | A, O | B, AB |
| B | B | Anti-A | B, O | A, AB |
| AB | AB | XX | A, B, AB, O | —– |
| O | XX | Anti-A&B | O | A, B, AB |
| Blood Group | Antigens (RH Factor) | Antibodies | Can Get Blood From | Cannot Get Blood From |
| +VE | X | -VE, +VE | X | |
| X | ||||
| -VE | X | Produce After Expose to RH Factor | -VE | +VE |
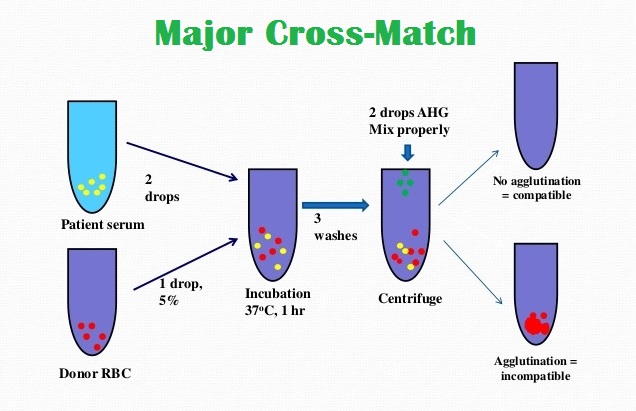
Major Cross Match:
In this test, the patient’s serum is mixed with the donor’s red cells. Laboratory group the patient and donor with Rh blood transfusions should be of the same group only. Earlier, group 0 was given to patients of any blood group, this practice is not correct. In this way, they used to give blood to AB people, this is also not appropriate, the blood transfusion should be of only one group.
First, mix about 0.5 ml of the donor’s blood with coconut saline in a test tube and fill the entire tube with coconut milk. After mixing, centrifuge for about 7-10 minutes. Remove the saline completely by repeating this process four times. This process is called the red cell washing process. After washing, make a 20% solution of this red cell with normal saline.
Collect the patient’s serum Serum should be very clean, do not use hemolyzed serum Perform direct antiglobulin and indirect antiglobulin tests on the patient’s serum This will know about the antibodies already present in the patient. Now take three small-sized tubes and add two drops of the patient’s serum and two drops of 200 red cells prepared by the donor inside each tube and mix it. Now proceed like this.
Keep tube 1 at room temperature, tube 2 and tube 3 in water hand at 37 degrees centigrade. Check all three tubes after fifteen minutes. After mixing, centrifuge for one minute, and if hemolysis and platelets are in the form of light granules, if this is not the case in all three tubes, discard the room temperature tube, tube two.
Add two drops of boudin albumin and incubate again at 37°C for ten minutes, then Take out the tube and look for Hemolysis and Agglutination and also examine under the microscope if either of these are present the blood will not be suitable for administration to the patient. Allow tube 3 to remain in the water bath at 37°C for another 30 minutes, then remove it.
Dash the red cells three times with saline again. Now mix two drops of anti-human globulin serum in it and check for agglutination after centrifugation, if it is not present and during all the previous factors, Hemolysis or formation of granules is observed under the microscope. If it is not seen, such blood can be given to the patient, but the cross-match of the donor is not enough, this blood should not be used without complete screening of the donor.
Donor Screening (Donor Selection):
Donating blood should be completely voluntary. Blood can be donated between the ages of 18-65 years. Yes, but the blood of pregnant women and lactating mothers cannot be taken.
Blood volume:
About 450 ml of one can be given at a time. The entire 450ml bag should not be taken from underweight individuals as there is a risk of fainting.
Donner Hemoglobin:
The hemoglobin of the donor should be checked before blood collection. Donors with hemoglobin less than 13.5 gm percent in men and 12.5 gm percent in women are not acceptable.
Bleeding interval:
Blood can be donated at most twice a year. Blood should never be taken from a professional donor.
Transfer of diseases:
Many diseases can be caused to the patient due to donor blood. Tests for these diseases are mandatory before giving blood to every donor.
Liver virus Test:
The B and C viruses are mainly well known and can infect the patient through the donor’s blood. Therefore, the HbsAg i.e. B virus test and the Anti-HCV i.e. C virus test must be done for every donor. Apart from B and C, some viruses can also do all this; they should also be tested. Sexually Transmitted Diseases eg Syphilis VDRL test should be mandatory for every donor. If positive, confirm with further tests. In case of confirmation, such a person should be prohibited from donating blood forever. These people can donate blood after complete treatment in case of malaria, etc.
HIV (AIDS) Test:
It is also called an HIV test. Nowadays, this disease is also spread by giving the blood of an AIDS patient to another person. Since this is a fatal disease that cannot be cured, every donor should be tested for AIDS and HIV. In case of being positive, the blood of such a person should not be taken at all, since drug addicts are common victims of this disease, the blood of drug addicts should not be taken. Also, blood should not be given to diabetics and kidney patients.


[…] is thought to be due to the patient forming antibodies against the white blood cells of the donor blood of donner plasma containing Leukoagglutinin antibodies it will react with the recipient’s white blood cells […]
You should take part in a contest for one of the best blogs on the web. I will recommend this site!
I conceive you have mentioned some very interesting points, regards for the post.
[…] SS Disease (HbSS): This is the most common and severe form of sickle cell anemia. Individuals with two copies of the HbS gene (one from each parent) have HbSS disease. These individuals experience frequent and severe pain crises, anemia, organ damage, and other […]